At CMC Joint Replacement Center, we understand how challenging life becomes when you live with chronic joint pain caused by arthritis, injuries or other conditions. When your ability to move and get around the way you used to be able to, becomes increasingly difficult and painful, you can turn to our Joint Replacement Center.
You might think joint pain is an inevitable part of aging, but it doesn’t have to be. Conway Medical Center has become the leader in life changing joint replacement surgery utilizing the latest advances in technology and pain management. With staff that is dedicated to assisting you through every step of your surgery we’ve put all the pieces together to help speed up recovery and get you back to the things you love.
We’re Here for You!
A Better Life is a Click Away.
What is Joint Pain?
Your knees, shoulders, elbows, and ankles are all joints that are susceptible to injury, damage, and pain. Pain from these joints usually stems from the damage of ligaments, tendons, cartilage bursae, and/or conjoining bones. Although joint pain is not usually a critical condition, it can severely limit a sufferer from mobility and performing daily tasks and activities. Joints allow our limbs and extremities to move freely, so it can be frustrating when those movements are restrained by pain.
Common Joint Pain Symptoms
While joint pain itself is a common symptom, there are numerous other effects that can come along with it. We can help our patients with symptoms like:
- Redness
- Swelling
- Tenderness
- Warmth
- Stiffness
- Weakness
- Limping
- Joint locking
- Limited range of motion of the joint
Joint Pain Causes
There are many reasons that joint pain develops, including:
- Arthritis, including Rheumatoid arthritis
- Bursitis
- Tendinitis
- Inflammation
- Gout
- Injury
Joint Pain Risks
Your daily routine may be putting you at risk for severe or chronic joint pain, These factors include:
- Obesity
- Smoking
- Higher Age
- Injuries due to work or athletic activity
- Stress and dissatisfaction with life
- Hard physical labor, especially involving repetitive action
Get back to an active lifestyle at our Joint Replacement Center
Patients who have total hip or total knee replacements typically recover quickly. You can expect to walk the day of your surgery. Most patients can safely go home the same day or the day after surgery. Generally, patients are able to return to driving in 2 to 4 weeks, go back to work in 6 to 8 weeks, and golf in 6 to 12 weeks. Your total joint team is dedicated to helping you return home and get back to the activities you enjoy.
Learn More About Joint Replacement
We provide the best care in our area, state, and nation







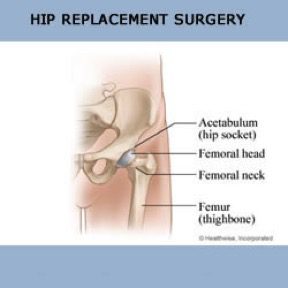
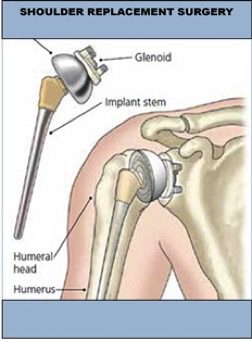
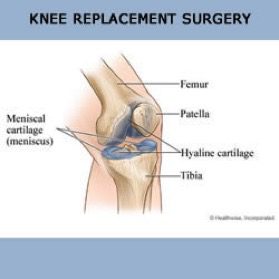 Patients frequently ask, “What exactly is a total knee replacement?” The simplest answer is that it is a replacement of the worn and arthritic surfaces of the knee joint. A total knee replacement resurfaces the worn parts of the joint. Unlike a hip replacement, that removes the ball of the hip joint, a total knee replacement takes away very little of the bone within the knee joint. It is better to think of a knee replacement as a refinishing of the knee surfaces. With arthritis, the cartilage covering the ends of the bone within the knee joint is badly worn. In a knee replacement this damaged cartilage, along with a very small amount of bone, is removed with very precise guides and instruments. The implants, which are made of metal and plastic in a variety of sizes, are then fitted to the bone to provide an artificial surface that causes no pain when the knee is in motion.
Patients frequently ask, “What exactly is a total knee replacement?” The simplest answer is that it is a replacement of the worn and arthritic surfaces of the knee joint. A total knee replacement resurfaces the worn parts of the joint. Unlike a hip replacement, that removes the ball of the hip joint, a total knee replacement takes away very little of the bone within the knee joint. It is better to think of a knee replacement as a refinishing of the knee surfaces. With arthritis, the cartilage covering the ends of the bone within the knee joint is badly worn. In a knee replacement this damaged cartilage, along with a very small amount of bone, is removed with very precise guides and instruments. The implants, which are made of metal and plastic in a variety of sizes, are then fitted to the bone to provide an artificial surface that causes no pain when the knee is in motion.